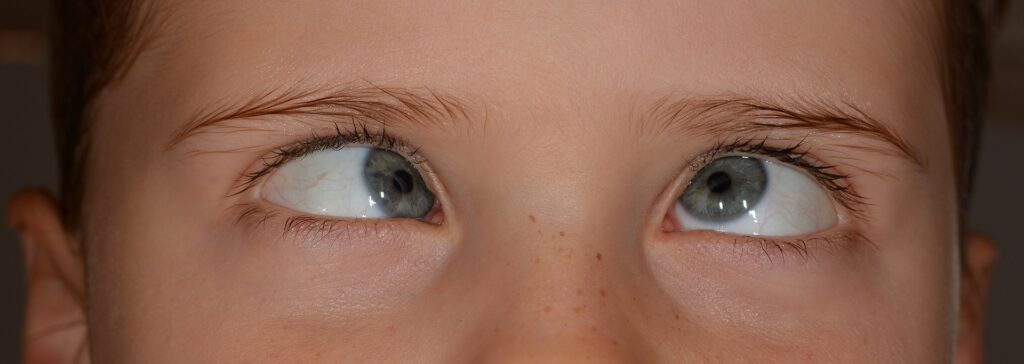
Orthoptics: My Child Is Squinting |
If your child has a squint, you will know that such sight dysfunction can significantly impact their development. Because 80% of all external stimuli are “received” via the sense of sight, a squint is a common, direct reason to be excluded from one’s peer group (the child fails to keep up with his/her peers) and to refrain from physical activity that requires proper visual perception and physical coordination. Luckily there are places, such as our orthoptic clinic, where parents can find help in the diagnosis and rehabilitation of squinting – so you can heave a sigh of relief!
orthoptics-my-child-is-squinting |
1. What is a squint?
A squint appears because of the non-parallel arrangement of the eyeballs when looking at an object. Only one eye is parallel with the line of sight while the other deviates at an angle.
orthoptics-my-child-is-squinting |
2. What are the symptoms of squinting?
The child looks straight ahead but one eyeball is turned in towards the nose or cheek. The picture they are looking at is unclear or blurred and may also be “double”, as squinting makes it difficult and sometimes impossible to form “fusion” – a process involving the joining of the two pictures received by each eye into one.
3. What are the direct reasons for the appearance of squints in children?
Reasons for squints in children:
• most often: non-adjusted or badly adjusted refraction disorders
• malfunctioning eyeball muscles.
Eye and nervous-system diseases as well as genetic factors can contribute to the development of a squint.
orthoptics-my-child-is-squinting |
4. What diagnostic methods are usually applied during an orthoptic diagnosis?
With each type of squint our certified orthoptist determines the extent of the visual impairment (i.e. refraction impairment). After accommodation paralysis induced by appropriate eye drops (Tropicamid, Atropine), which “paralyses” the accommodation mechanism painlessly, the orthoptist will conduct an objective refraction test.
orthoptics-my-child-is-squinting |
5. What are the ways of correcting a squint?
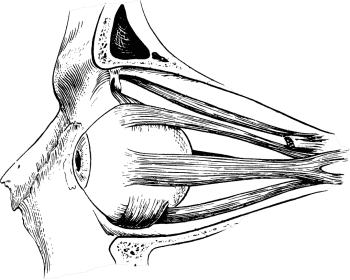
If the squint is caused by visual impairment the child must wear appropriate corrective glasses. Sometimes ophthalmologists/ certified orthoptists advise covering the healthy eye with a plaster or a blindfold (so-called obstruction). Treatment is often supported with eyeball training – orthoptic exercises. If surgery is necessary to restore muscle balance it can be performed around the 4th year of the child’s life. The surgery will weaken the functioning of the muscle that draws the eye too tightly in one direction while strengthening the other one, which is too weak.
orthoptics-my-child-is-squinting |
orthoptics-my-child-is-squinting |
6. What is orthoptic therapy?
Orthoptic exercises aim at reducing the angle of the squint and making binocular vision more efficient. Therapy consists of a gradual and long-term process, sometimes even over many years. It requires a lot of patience and smooth cooperation between the child and the orthoptist. At a further stage of rehabilitation parents play a significant role as very often such therapy must be continued at home. It doesn’t matter whether the squint is hidden or not – it doesn’t pass spontaneously; it always requires treatment! Treatment before the child starts education at school is preferred, as physiological binocular vision forms at around the 7th year of life.
orthoptics-my-child-is-squinting |
Let’s see how the FUSION EXERCISE looks like:

orthoptics-my-child-is-squinting |
7. How can a squint make a child’s every-day life difficult?
A child who suffers from a squint has difficulties in recognising shapes, catching toys or even crawling. They are not able to assess distance appropriately, so you should notice very early on that they will run into small objects and bump into larger objects standing in their way. Not only can this result in bruising but it can also be a permanent detriment to health!
orthoptics-my-child-is-squinting |
8. What should you take into account if you notice alarming symptoms?
Start a little revolution with the decoration of your home! Objects placed directly on the floor (large plants, vases with artificial flowers, dumbbells, electronic gadgets – such as the PlayStation, stools, stands, shoes etc.) should be put in places to which a child has no access. Organising space in such a way that it is not a danger for your child is very important and even crucial, especially in the case of a child who suffers from a squint.
9. Is an untreated squint a threat to my child?
Yes, irrespective of the level of advancement, a squint is always a threat to the functioning of the optic system, and the child should be treated by an orthoptist without any delay. An untreated squint may lead to the visual impairment of the eye, as images forming in the wrong part of the retina will be muffled in order to avoid binocular vision.
orthoptics-my-child-is-squinting |
10. Does early diagnosis of a squint increase the chances of elimination?
You need to be aware of the fact that a child does not “grow out” of a squint and it will not disappear! Thus, the sooner the irregularity in the child’s vision is diagnosed and therapy started the better! This illness applies to 2-5% of all children and constitutes one of the major reasons for psychological complications which have an impact on results in education and behavioural problems. Why is time a crucial issue? The older the child, the fewer the chances for full recovery. In the case of younger children we can more efficiently treat the formation of binocular vision, and the treatment has a better effect. Despite the fact that such therapy may take even a few years, full recovery is guaranteed.
11. What different types of squint are there?
There are several types:
a) pseudostrabismus – a condition caused by the non-parallel arrangement of the eyeballs, damage to the eye’s protective apparatus, and in small children – in the majority of cases – a small distance between the pupils or a wide nasal bridge, a so-called epicanthic fold;
b) heterophoria, strabismus latens – usually appears periodically and not permanently; it takes effect in visible eye variance, which arises as a result of atrophy (interruption) of binocular vision (fusion stimuli); it manifests itself through he malfunctioning of the muscles in the eyeballs that keep them in the correct position – it is most often connected with muscle balance disorder. Common symptoms are: eye fatigue, headaches, blurred vision, double vision and conjunctivitis (so called asthenopia symptoms);
c) tropia, strabismus, heterotropia – a hidden squint may transform into stabismus if diagnosed too late and if appropriate therapy is not applied. Other reasons for the appearance of strabismus include: unaligned refraction disorder (sight defect), anisometropia, temporary eye cover, mental or physical shock, virus infection or bacterial infection of the eye;
d) strabismus paraliticus – this can appear as a result of the paralysis of one of the cranial nerves which provide innervations to one of the six outer ocular muscles moving the eye ball; it manifests itself as double vision and eye movement disability as to the direction in which a given muscle operates.
There are few others types of squint: accommodative strabismus, downwards strabismus, upwards strabismus, severe strabismus, vertical strabismus, discrepant strabismus (+ hidden discrepant strabismus), diagonal strabismus, convergent strabismus (+ infants’ convergent strabismus).
12. What are the types of squint that depend on the direction of eyeball variance towards the optical axis?
Types of squint that depend on the direction of eye variance: convergent, diagonal, vertical or discrepant.
We invite you to register for a check up with the children’s ophthalmologist and an orthoptic diagnosis with our certified orthoptist. Contact us on 22 266 09 95. Or write to us at biuro@zobaczycjutro.org. Our Children’s Eye Center is the most children-friendly place in Warsaw!



Najnowsze komentarze